April 1, 2026
Addressing the complex nature of pain management and its relationship to healing. Understanding the depth and breadth of pain is essential for devising effective pain management treatments that facilitate healing. Pain is multifaceted, driving the need for a nuanced approach to treatment, and involves both physiological and psychological dimensions. Traditional management techniques often rely on pharmaceuticals, which play a crucial role but may not address the root causes or comprehensive recovery.
1. Understanding Pain: Types and Causes
1.1. Acute Pain vs. Chronic Pain
Pain is primarily categorized into acute and chronic types, each necessitating distinct approaches to management and treatment. Acute pain arises suddenly and is typically associated with a specific injury or illness, acting as a warning signal to potential harm. In contrast, chronic pain persists beyond the usual recovery period, often lasting for months or even years, and can be exacerbated by psychological factors. According to the Center of Disease Control (CDC), women were more likely to have chronic pain (25.4%) and high-impact chronic pain (9.6%) than men (23.2% and 7.3%, respectively), underscoring the prevalence and impact of chronic pain. The management of chronic pain poses a significant challenge due to its complex nature and implications on daily life. Pain management treatments must be tailored specifically to each individual's needs.
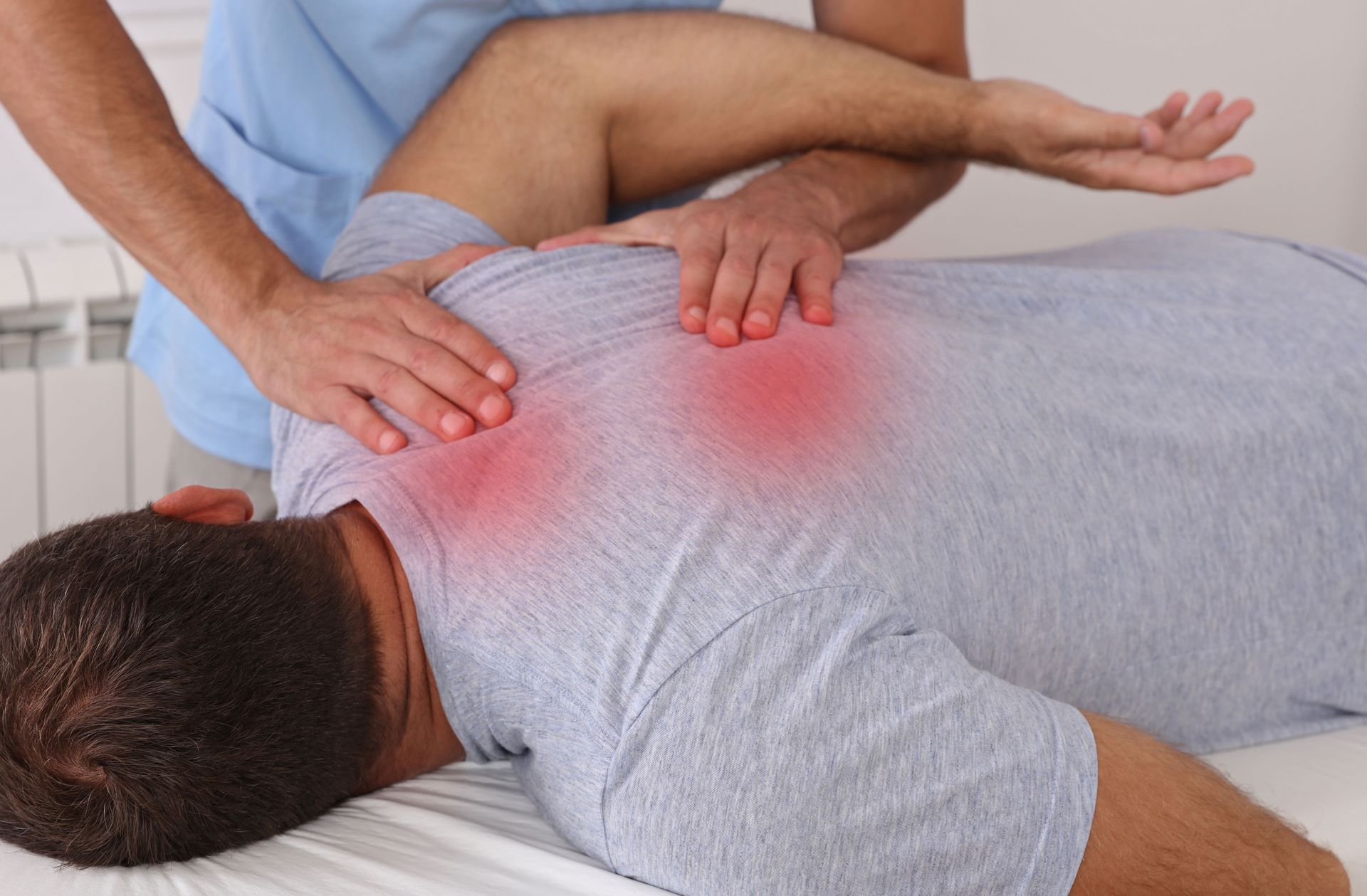
1.2. Sources of Inflammation
Inflammation is an integral process of the body's immune response, though it can lead to pain when left unchecked or chronic. Common sources of inflammation include infections, injuries, and autoimmune disorders, each contributing to pain through different mechanisms. While acute inflammation is typically protective, chronic inflammation can result in tissue damage and might require outside intervention for resolution. Understanding these sources is crucial in targeting treatments that address both the inflammation and the resultant pain effectively. Identifying and mitigating these sources helps in crafting comprehensive pain management strategies that align with individual needs.
1.3. Neuropathic Pain Origins
Neuropathic pain results from damage or dysfunction of the nervous system, manifesting as sharp, burning sensations often coupled with tingling and numbness. Conditions such as diabetes, multiple sclerosis, and post-surgical nerve damage can cause neuropathic pain, which is notoriously challenging to treat. Unlike nociceptive pain caused by physical damage, neuropathic pain does not respond well to standard painkillers, making targeted treatments crucial. An understanding of the origins of neuropathic pain is imperative for developing interventions that aim to diminish these distressing symptoms. Innovative approaches such as neuromodulation are becoming increasingly relevant in addressing this category of pain effectively.
1.4. Impact of Psychological Factors
Pain is not solely a physical phenomenon; psychological factors can significantly influence both the perception and management of pain. Stress, anxiety, and depression can exacerbate pain perception and diminish quality of life for those afflicted. The mind-body connection is evident in the realm of pain management, with psychological interventions proving beneficial alongside traditional medical treatments. Understanding the psychological dimensions is essential in tailoring therapies that not only alleviate physical symptoms but also address mental well-being. Techniques such as cognitive behavioral therapy have become integral in comprehensive pain management treatments.
2. Natural and Alternative Remedies
2.1. Herbal Supplements With Anti-inflammatory Benefits
Herbal supplements such as turmeric, ginger, and boswellia are popular natural options for managing inflammation and associated pain. These supplements contain active compounds that reduce inflammatory markers and support the body's healing processes. While generally well-tolerated, potential interactions with medications necessitate cautious and informed use. Incorporating herbal supplements into pain management plans offers a complementary approach to pharmaceutical treatments.
2.2. Role of Diet in Reducing Inflammation
A diet rich in anti-inflammatory foods can significantly impact pain management by addressing the underlying causes of inflammation. Foods such as fish, nuts, fruits, and leafy greens contain nutrients that modulate inflammatory processes and promote overall health. Avoiding processed foods and excessive sugars further supports these dietary efforts, reducing pro-inflammatory stimuli. Educating patients on nutritional choices enhances their ability to manage pain through lifestyle modifications. A well-rounded diet is integral in fostering healing and long-term pain relief.
2.3 Importance of Rest and Immobilization
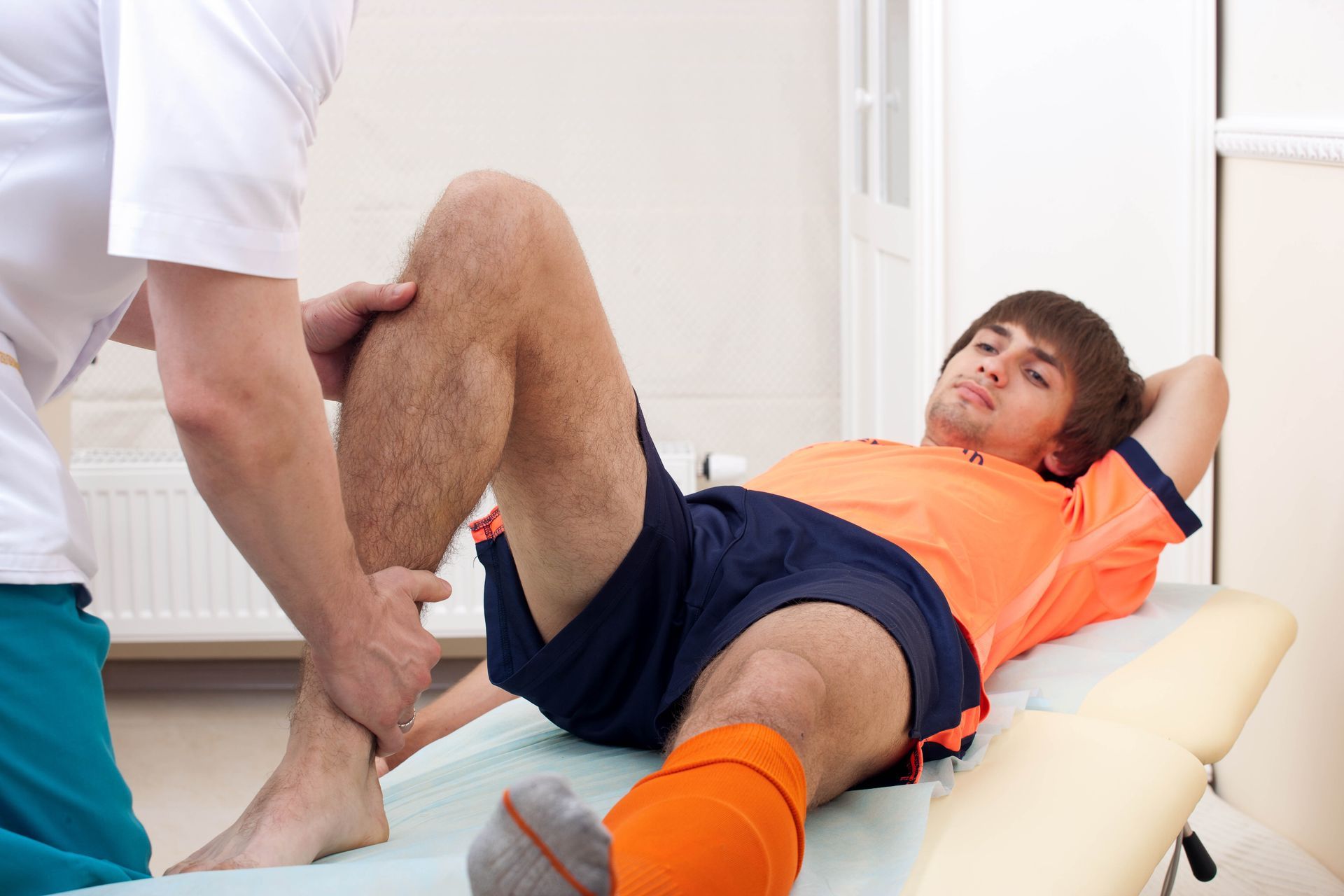
Rest and immobilization are often critical in the initial stages of injury management, allowing the body time to repair damaged tissues. While prolonged inactivity can lead to stiffness and muscle atrophy, the strategic use of rest is essential in preventing further injury and facilitating healing processes. Clinical guidance is invaluable in determining appropriate rest periods and the timing of reintegration of activity. Graduated return to movement is crucial, balancing healing needs with maintaining strength and mobility.
3. Advanced Medical Interventions
3.1 Image-Guided Biologic Injections
Image-guided biologic injections are an advanced approach in pain management that combines precision medicine with regenerative therapies. Using real-time imaging technologies such as ultrasound or fluoroscopy, physicians can accurately locate the damaged tissue or joint requiring treatment. This precision ensures that biologic agents—like platelet-rich plasma (PRP) or stem cells—are delivered exactly where they are needed, maximizing effectiveness and minimizing the risk of injury to surrounding tissues. PRP injections utilize the patient’s own blood, concentrated with healing factors, to stimulate tissue repair and reduce inflammation. Stem cell injections can promote regeneration of cartilage, ligaments, or tendons, potentially restoring function in areas damaged by injury or chronic conditions. Patients receiving these injections often report faster recovery, improved mobility, and reduced reliance on pain medications compared to traditional corticosteroid injections. This therapy is particularly valuable for conditions such as osteoarthritis, tendon injuries, and joint degeneration, offering a minimally invasive option that targets the root cause rather than just masking symptoms.
3.2 MLS Laser Therapy
Multiwave Locked System (MLS) laser therapy is a non-invasive treatment that uses a combination of synchronized laser wavelengths to reduce pain and accelerate healing. The therapy works by stimulating cellular activity, improving blood flow, and decreasing inflammation in the targeted area. MLS laser therapy is effective for a wide range of conditions, including musculoskeletal disorders, soft tissue injuries, post-surgical recovery, and chronic pain syndromes. One of the key benefits of MLS therapy is that it addresses both the pain and the underlying inflammation, helping tissues repair more efficiently. The treatment is painless, safe, and can be repeated as needed without harmful side effects. Patients often notice reduced swelling, improved mobility, and shorter recovery times after consistent sessions. MLS laser therapy can also reduce the need for oral medications or invasive procedures, making it an excellent option for patients seeking a conservative yet effective solution to chronic or acute pain.
3.3 Combination Therapies for Optimal Recovery
Combining treatments such as image-guided biologic injections with MLS laser therapy offers a comprehensive, multi-modal approach to pain management. While biologic injections promote tissue regeneration and repair at the cellular level, MLS laser therapy enhances blood flow, reduces inflammation, and accelerates healing in surrounding tissues. Together, these therapies can provide more consistent and longer-lasting pain relief than either treatment alone. This combination approach is especially useful for complex injuries or chronic conditions where a single intervention may not be sufficient. By integrating multiple treatment modalities, healthcare providers can customize therapy plans to the patient’s specific needs, taking into account the type of injury, severity, and overall health. The result is improved function, faster recovery, and a higher quality of life for patients, with reduced dependence on medications or more invasive procedures.
Effective pain management treatments require a comprehensive and nuanced approach that addresses both the physical and psychological dimensions of pain. Incorporating lifestyle changes, diet, and non-pharmacological therapies further supports long-term recovery and overall well-being. For more information, contact Palm Beach Regenerative Sport and Spine today.